Maternal, Early Childhood Health & Survival

Cold Chain Storage
Led by: Maria Drangova
Partner(s): Makarere University, Uganda; Drop Access, Kenya
Technology Summary: This technology transforms widely available 12 V camping refrigerators into validated, medical-grade cold storage systems for vaccines and other temperature-sensitive medications. By integrating optimized solar panels, battery systems and continuous temperature monitoring, the units maintain the World Health Organization’s required 2–8 °C range — even in off-grid settings. The result is a reliable, low-cost cold chain solution built from mass-produced consumer equipment and re-engineered for global health impact.
Who it's for: This technology is designed for health clinics and community health providers in remote and low-resource settings where electricity is unreliable or unavailable. It supports families and patients who rely on consistent access to life-saving vaccines and medications.
See also: PhD Candidate, Kato Hussein Wabbi (Frugal Edge AI-Base Predictive Maintenance System)
Open-Source Jaundice Phototherapy Devices
Light calibration system
Led by: Joshua Pearce
Partner(s): Kenyatta University, Kenya
Technology Summary: This project developed a low-cost, open-source light sensor that calibrates phototherapy devices used to treat neonatal jaundice (hyperbilirubinemia). Built using distributed manufacturing and 3D printing, the device accurately measures light intensity and wavelength to ensure infants receive safe and effective treatment. Validated against a commercial Ocean Insight UV-VIS spectrometer and hospital phototherapy systems such as the Datex-Ohmeda Giraffe Spot PT Lite, it delivers 98.6% accuracy at a cost of under US$150.
Related publications: Open-source light calibration system
Who it's for: This technology is designed for hospitals and neonatal care units in low- and middle-income countries that use low-cost phototherapy systems but lack affordable tools to properly calibrate them. It helps clinicians safely treat newborns with jaundice while expanding access to life-saving care.

Low-cost light therapy device (jaundince treatment)
Led by: Joshue Pearce
Partner(s): Kenyatta University, Kenya
Technology Summary: This project developed a low-cost, open-source neonatal phototherapy device (NPTD) to treat severe neonatal jaundice. The device was designed, built, and validated to meet international clinical standards (American Academy of Pediatrics and UNICEF). Despite costing roughly one-tenth the price of commercial alternatives, it delivers equal or better treatment performance, including appropriate light wavelength, high irradiance, and uniform light distribution. Because it is open-source, the full design can be freely accessed, built, and adapted, enabling scalable and reliable treatment in a wide range of settings.
Related publications: Neonatal Phototherapy Device
Who it's for: This technology is intended for healthcare providers working in low- and middle-income countries, particularly in resource-limited hospitals and clinics that cannot afford traditional phototherapy equipment. It ultimately serves newborns at risk of severe jaundice.
Malaria Diagnostics
Loop-Mediated Isothermal Amplification (LAMP) System
Led by: Kibret Mequanint
Partner(s): Tropical and Infectious Disease Research Centre (TIDRC), Ethiopia; Jimma Institute of Technology (JIT), Ethiopia
Technology Summary: This project is developing a low-cost, battery-powered LAMP (Loop-Mediated Isothermal Amplification) device to detect and quantify malaria parasites in low-resource settings. Designed for use in rural clinics with unreliable electricity, the system operates at room temperature, delivers rapid results, and automates interpretation to reduce human error. By combining affordability, portability, and accurate quantification, the device aims to strengthen early diagnosis and treatment in regions most affected by malaria.
Who it's for: This technology is designed for frontline health workers and rural clinics in malaria-endemic regions, particularly across sub-Saharan Africa. It supports timely, accurate diagnosis in communities where conventional laboratory testing is inaccessible or unaffordable.
See also: PhD Candidate, Etagegnehu Dagnachew Feleke (Low-Cost Loop-Medicated Isothermal Amplification (LAMP) System for Malaria Diagnosis
Neonatal Brain Oxygen Monitoring
Led by: Mamadou Diop
Partner(s): University Cheikh Anta Diop (UCAD), Senegal
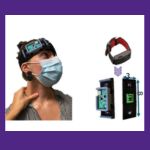
Technology Summary: This project developed a low-cost, wearable near-infrared spectroscopy (NIRS) device to monitor cerebral blood oxygenation in newborns at risk of brain injury. Built using widely available consumer electronics, the system measures changes in oxygenated and deoxygenated hemoglobin in real time using dual-wavelength light. Designed specifically for low-resource settings, the device offers a noninvasive, portable solution for early detection of neonatal brain injury.
Who it's for: This technology is intended for neonatal units and frontline health providers in underserved and low-resource regions where advanced neuromonitoring tools are unavailable. It supports earlier detection and intervention for infants at risk of brain injury due to infection, malnutrition, or other complications.
Publications: Wearable near-infrared spectroscopy device for low-resource settings
Non-invasive Blood Testing
Led by: Michael Rieder
Partner(s): Cissy Kityo, Joint Clinical Research Centre, Uganda; BioNext Medical Innovators Hub (Robarts Research)
Technology Summary: This project is developing a non-invasive system that determines blood cell counts in real time by capturing and analyzing images of light directed through the capillary nailbed. Using single-cell imaging and advanced image analysis, the technology aims to eliminate the need for traditional blood draws and laboratory testing. The device integrates hardware and software to deliver point-of-care blood analysis in a portable format.
Who it's for: This technology is designed for health-care providers working in rural, remote, and resource-constrained settings who need immediate blood count information to guide diagnosis and treatment. It supports faster clinical decision-making without relying on laboratory infrastructure.
Oral Health Prevention, Diagnosis & Tele-dentistry
Led by: James Lacefield and Noha Gomaa
Partner(s): University of Nairobi, Kenya
Technology Summary: We are developing technologies to improve detection of oral health conditions in communities that have limited access to dentistry services. These technologies include a color-changing paper strip to detect white blood cells in saliva that are indicative of gum disease and a low-cost intraoral camera with AI-based image analysis software to detect early-stage cavities. The intraoral camera will be a key component of a cost-effective tele-dentistry system that will enable dentists to provide diagnostic services remotely to patients in rural and remote clinics. We are also developing a low-cost gamified smart toothbrush for children that will encourage them to be attentive to proper brushing techniques.
Who it's for: The colorimetric strip and the intraoral camera will enable non-specialist healthcare providers in small local clinics to provide basic oral health care to their communities and identify patients who should be referred for dental care at larger centres. The smart toothbrush is intended for home use, particularly among children with neurodevelopmental challenges who can struggle with establishing good brushing habits.
See also: MESc Candidate, Sirui Gao (Low-Cost Intraoral Camera & Tele-Dentistry System)